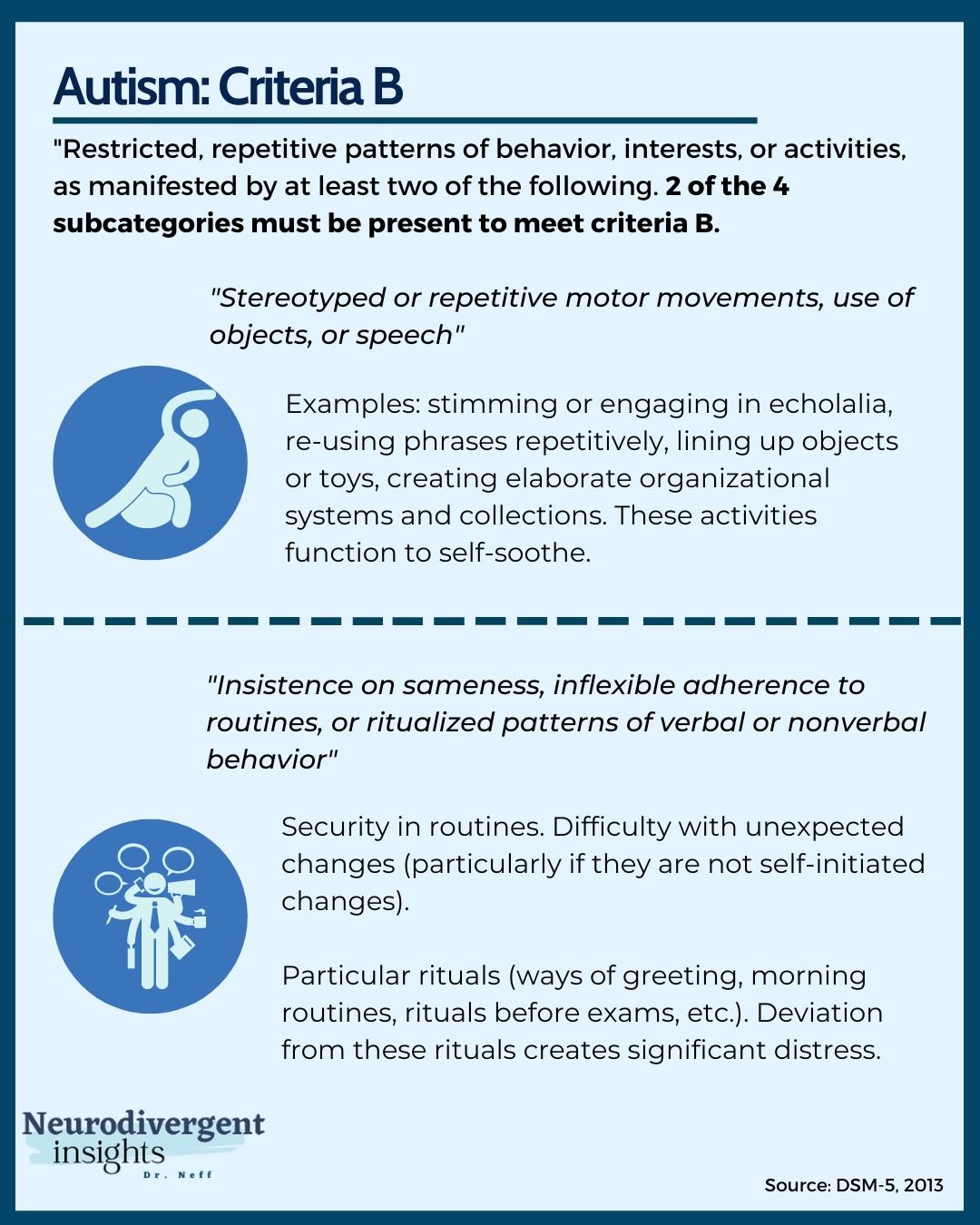
Ideally, treatment recommendations are evidence-based, but personalized through knowledge of each patient’s unique needs.Ĭomorbidity should be suspected when core features fail to explain impairment, when there is noticeable change from baseline, or when the patient is not responding to therapeutic interventions as expected. A reliable developmental history, family history, comprehensive phenotype of the patient, and functional behavioral assessment of target symptoms are necessary to develop effective, well-tolerated therapeutic interventions that would lead to sustained overall improvement. The lack of gold standard instruments to assess comorbidity may explain the wide range of findings regarding prevalence and outcomes. Semi-structured, interviewer-rated tools, such as the Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I) performed by a clinician experienced in the field of autism may be more valid than highly structured responder-dependent tools. The newly available Anxiety Scale for Children - ASD, Parent and Child versions (ASC-ASD) shows promise. The Autism Comorbidity Interview-Present and Lifetime version (ACI-PL), Children’s Interview for Psychiatric Syndromes-Parent version (P-ChIPS) and, Children's Yale- Brown Obsessive Compulsive Scale (CY-BOCS) modified for ASD are some helpful tools. In order to reduce diagnostic complexity and develop consensus interventions, validated scales to investigate comorbidity are needed. Finally, environmental factors and stressors may alter both core symptoms and comorbidity phenotype. The comorbidity may be further modified by the severity of core symptoms and degree of intellectual disability. The phenotype of comorbidities may differ from the disorder outside of the context of ASD. Separately, core features and comorbidities may have overlapping symptoms, obscuring the comorbidity. Distinct genetic syndromes may also underlie heterogeneous presentations. The affected person may not be able gauge the impact of their own behavior on others. The identification of psychiatric comorbidity remains a significant challenge for clinicians: The nature of ASD makes it difficult to assess thoughts and emotions for reasons that include impaired reciprocity in the conversational process, difficulty identifying emotions, impaired theory of mind, and lack of empathy. 
Identifying such targets for treatment can certainly improve overall patient functioning and family wellbeing. The research evidence for symptomatic relief in ASD outside of core symptoms has grown substantially in recent years. Īdvances in genetics and neuroscience have led to the identification of promising target molecules and neurophysiological pathways involved in ASD. These impairments are outside of the core diagnostic symptoms of communication and social skills deficits, and restrictive interest / repetitive movements nevertheless, they are associated with significant impact and may impede the implementation of behavioral or other non-medical interventions. This article addresses the assessment and management of several symptoms or syndromes that significantly interfere with adjustment and functioning in individuals with ASD. A less studied source of impairment in Autism Spectrum Disorders (ASD) relates to psychiatric comorbidity. Lifelong functional impairment related to core autism features, such as social and communication deficits are well documented. 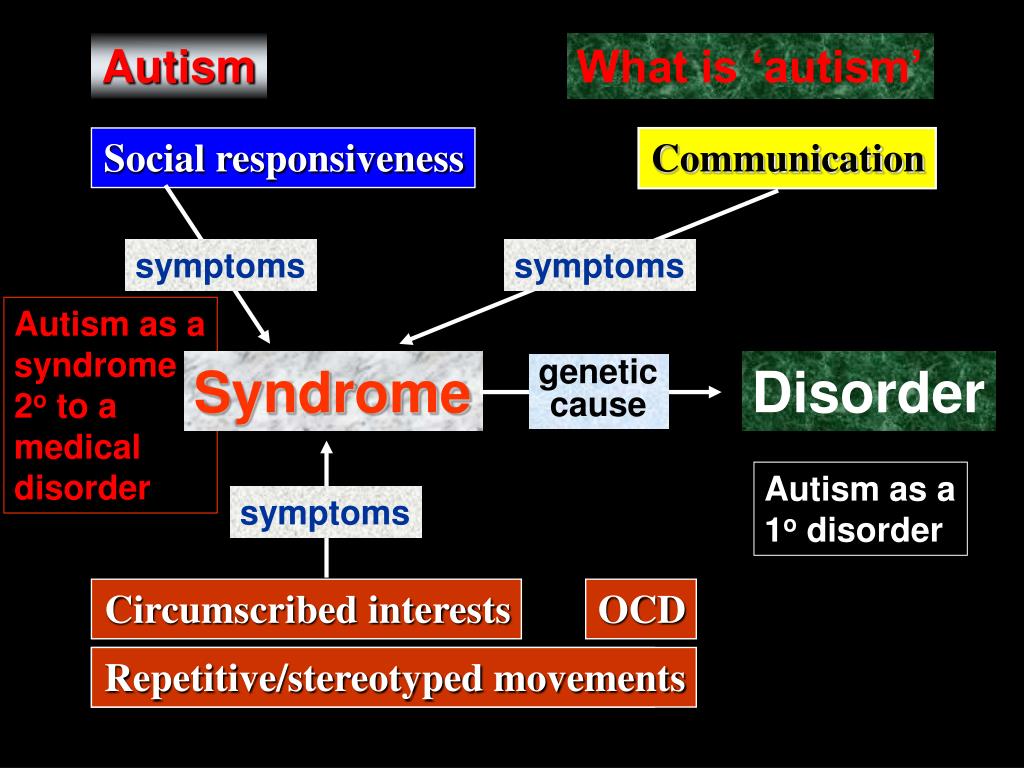
Autism spectrum disorder Asperger disorder Comorbidity Treatment Introduction
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
